ACO Strategy
Support for designing, joining, and optimizing ACO and value-based care arrangements, including attributed population analysis, shared savings modeling, quality tracking, and network planning tailored to rural FQHC realities.
HealthFront Ventures helps rural Arizona FQHCs evaluate, design, and operationalize value-based payment models with data-driven strategy, claims insight, and measurable performance frameworks. From Medicaid realities and county-level access gaps to workforce constraints common across frontier communities, this page outlines practical services that support sustainable reimbursement and stronger care outcomes.

Strategic, analytic, and measurement services built to help rural FQHCs succeed under value-based reimbursement.
Support for designing, joining, and optimizing ACO and value-based care arrangements, including attributed population analysis, shared savings modeling, quality tracking, and network planning tailored to rural FQHC realities.
Multi-payer claims analysis across Medicare, Medicaid, and commercial data to identify utilization patterns, access gaps, payer mix, and reimbursement opportunities that shape stronger value-based payment decisions.
Program design services that connect clinical quality, access, and outcomes to compensation and contract structures through scorecards, benchmarks, incentive models, and improvement roadmaps.
County-level workforce diagnostics that map physician and NP/PA shortages, helping FQHCs align payment reform with staffing realities, access barriers, and priority intervention areas.
Quantitative measurement and reporting aligned with CMS Rural Health Transformation requirements, producing audit-ready reports on access, utilization, quality, workforce expansion, and sustainability.
AI-native outsourced data warehouse and lake services that give rural organizations a practical foundation for claims integration, provider analytics, and ongoing value-based performance management.
Value-based payment works best when reimbursement design reflects real operating conditions. HealthFront Ventures helps rural Arizona FQHCs connect claims data, workforce capacity, quality measures, and access patterns into practical payment strategies. Whether your organization is evaluating ACO participation, Medicaid-aligned incentives, or performance-based contracts across sparsely populated counties, the goal is clearer measurement, stronger financial sustainability, and better patient outcomes.
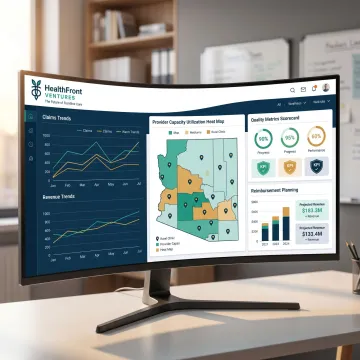
HealthFront Ventures combines rural healthcare strategy with practical analytics built for execution.
Built specifically for rural providers, with models suited to Arizona's dispersed counties and access constraints.
Outsourced AI-native data infrastructure reduces internal build burden and speeds reimbursement analytics readiness.
Performance frameworks tie quality, access, and outcomes to contracts with clear benchmarks.
From CMS-aligned measurement to workforce planning, guidance supports practical rollout across rural Arizona FQHC operations.
Focused expertise for rural healthcare transformation.
HealthFront Ventures is focused on transforming rural healthcare through data-driven workforce and reimbursement solutions. The company is evolving from RHT NOFO submission support into state-level RHT execution services, with an emphasis on practical analytics, measurable outcomes, and outsourced infrastructure that reduces complexity for clients. For rural Arizona FQHCs, that means support shaped around frontier access challenges, Medicaid-heavy payer environments, and county-level workforce shortages that can directly affect payment model success. HealthFront Ventures positions its work around AI-native workforce data warehouses, claims intelligence, and performance measurement frameworks that help organizations move from fragmented reporting toward sustainable value-based strategy and operational execution.
ACO payment models generally include shared savings only, shared savings with downside risk, and more advanced population-based arrangements. For rural FQHCs, the right model depends on attributed lives, quality reporting capacity, payer mix, and financial tolerance. A practical evaluation should review benchmark methodology, care management requirements, network adequacy, and whether the organization has enough claims and workforce visibility to manage performance reliably.
Talk with our team about strategy, analytics, and rural execution.
Certified outsourced analytics-ready workforce foundation.
Certified support for quantitative program reporting.
Certified focus on MD and NP/PA data.
Share your reimbursement goals, reporting needs, or rural market challenges, and we'll outline how our strategy and analytics services can support your organization.
To help us assist you faster, please include the reason for your message so the relevant team can reach out as soon as possible.
To help us assist you faster, please include the reason for your message so the relevant team can reach out as soon as possible.