
Introduction
Roughly 20% of Americans live in rural areas, yet only 10% of physicians practice there — a 2:1 population-to-physician mismatch that represents an operational threat to hospital viability. With 199 rural counties having zero primary care physicians and the projected shortage reaching 70,610 FTE primary care physicians by 2038, rural hospitals face recruitment challenges that go far beyond filling current vacancies.
This guide provides a practical, strategic roadmap for rural hospital administrators and health program directors. You'll learn how to:
- Structure competitive compensation packages with loan repayment and retention bonuses
- Build professional environments that offer autonomy and collaborative staffing
- Create community partnerships that address spousal employment and quality-of-life concerns
- Access underutilized government programs like NHSC and Conrad 30
The goal is a sustainable physician recruitment approach built on data, not guesswork.
TLDR
- The rural physician gap is structural and worsening — one-off job postings won't close it
- Competitive packages must combine base salary, loan repayment, retention bonuses, and housing support
- Physicians weigh scope of practice, autonomy, community fit, and spousal employment as heavily as pay
- Before any search begins, baseline workforce data — ratios, vacancy patterns, turnover — should set your recruitment targets
- Most rural hospitals leave NHSC, Conrad 30, and HPSA designation on the table — programs that expand candidate pools and cut financial barriers significantly
Why Rural Physician Recruitment Is Getting Harder
The rural physician shortage isn't cyclical — it's structural. HRSA projects nonmetro areas will reach only 61% supply adequacy versus 83% in metro areas by 2038, with the total national shortage reaching 141,160 FTE physicians. The AAMC's 2036 forecast puts the gap at up to 86,000 physicians — and both agencies agree rural areas will absorb the worst of it.
The distribution problem is severe, not just the total count:
- 92% of rural counties are designated primary care HPSAs, compared to 83% of urban counties
- 45% of rural counties have five or fewer primary care physicians
- The rural average is 1 physician per 2,881 residents, dropping to 1 per 3,411 in the South
- States like Mississippi, Utah, and Idaho have fewer than 76 primary care physicians per 100,000 population
This shortage is also self-accelerating. Over 50% of rural physicians are aged 50 or older, meaning retirements will outpace what training pipelines can replace.
Burnout intensifies the problem. At 45.2% nationally, physician burnout hits harder in rural settings — professional isolation, heavier call burdens, and no specialist backup create conditions that push providers out faster than they can be replaced.
Those workforce pressures translate directly into hospital closures. Since 2010, 152 rural hospitals have closed or converted, and physician shortages are a consistent factor in financial collapse. Each primary care physician generates approximately $1.4 million in labor income and supports 26.3 jobs — meaning every unfilled vacancy carries real financial risk for the entire community the hospital serves.

Strategic Planning: The Foundation Before You Recruit
Successful recruitment isn't about filling a vacancy — it's about making the right long-term match. The pre-recruitment checklist should include:
Recruiting for Retention Framework
- Assess community need through gap analysis and service line priorities
- Form a recruitment committee with clinical, administrative, and community representation
- Budget explicitly for retention (not just hiring costs)
- Evaluate first-impression factors: website quality, responsiveness, site visit execution
Build a Comprehensive Candidate Profile
Go beyond clinical qualifications. Include lifestyle and community fit factors: desired region, preferred town size, outdoor or cultural amenities, school quality, and spousal employment opportunities.
Spousal employment ranks among the top three retention drivers, alongside community fit and professional autonomy. Interviewing a candidate's spouse or partner — where applicable — is a recognized best practice, because family satisfaction predicts retention as strongly as physician satisfaction.
Establish Baseline Workforce Data
Before launching a recruitment campaign, know your current HCP-to-population ratios, average vacancy duration, and turnover patterns. This measurable baseline lets you set realistic targets, prioritize specialty gaps, and track progress over time.
Tools like HealthFront Baseline™ provide rural organizations with these metrics directly — so you can make informed decisions about where to recruit first rather than defaulting to whoever applies.
Community Infrastructure Reality Check
58% of rural populations live in childcare deserts compared to 44% in urban areas. Address this barrier proactively by identifying childcare resources, spousal employment partnerships, and school quality data before candidates visit.
Building a Competitive Compensation Package
Even organizations with compelling community stories will lose candidates if the financial package doesn't clear a basic threshold. Compensation must lead — but transparency matters as much as the total number.
Base Salary Calibration:
Research current benchmarks through MGMA or Medscape data. Primary care physician earnings rose 3.9% year-over-year in the 2025 Medscape report, while specialist earnings rose only 2.4%. The rural-urban compensation gap may be smaller than candidates assume — communicate this clearly in job postings to avoid self-selection bias.
Structured Financial Components:
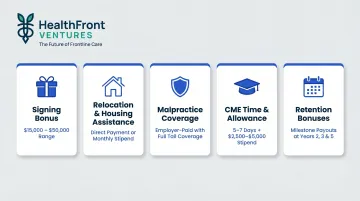
| Component | Purpose | Structure |
|---|---|---|
| Signing bonus | Immediate financial incentive | One-time, typically $15,000-$50,000 depending on specialty |
| Relocation/housing assistance | Reduce financial barriers to moving | Direct payment or stipend; consider ongoing housing support |
| Malpractice coverage | Remove financial risk | Employer-paid, tail coverage included |
| Paid CME time | Professional development | 5-7 days annually plus stipend ($2,500-$5,000) |
| Retention bonuses | Long-term commitment incentive | Structured at 2-, 3-, and 5-year milestones |
Student Loan Repayment as a Top-Tier Incentive:
The median medical school debt for the Class of 2024 is $205,000, with 63% of graduates planning to enter loan forgiveness programs. Offering structured loan repayment — whether employer-funded or through coordination with federal programs — improves offer acceptance rates, particularly for younger candidates. For early-career physicians carrying six-figure debt, loan repayment often outweighs base salary differences when comparing offers.
Quality Incentive Programs:
Where loan repayment addresses financial security, quality-based bonuses appeal to a different motivation: physicians who want their compensation to reflect the impact of their work. Tie performance bonuses to specific, achievable targets rather than vague quality goals — for example:
- Patient satisfaction scores
- Preventive care completion rates
- Chronic disease management metrics
Compensation Transparency:
Be upfront about the full financial package — base salary, bonuses, benefits dollar value, and loan repayment value — in job postings. Vague language like "competitive compensation" produces fewer qualified applicants and extends the hiring timeline. Candidates who see a complete, itemized offer move through the decision process faster — and with fewer competing offers to consider.
Creating a Professional Environment That Attracts and Retains
Compensation gets candidates to the table. Professional environment keeps them there.
Physician Autonomy as a Recruitment Asset:
Rural physicians often have broader scope of practice and fewer administrative layers than urban counterparts. Frame this authentically as clinical freedom, decision-making authority, and opportunity for leadership. Don't gloss over it — make it a centerpiece of your recruitment message. Physicians motivated by autonomy will self-select in; those who prefer highly structured hierarchies will self-select out.
Collaborative Care Models Using APPs:
HRSA projects that nurse practitioner supply in rural areas will exceed demand, creating an opportunity to build collaborative staffing models. Expanding your NP/PA workforce:
- Distributes on-call responsibilities across more providers
- Reduces burnout risk by sharing patient volume
- Improves work-life balance for physicians
- Makes physician roles more attractive by reducing routine task burden
Collaborative staffing is a retention strategy that makes rural practice sustainable — and positions rural roles as genuinely desirable, not just available.
Telemedicine Infrastructure:
Strong telehealth capabilities serve dual purposes: expanding patient access and reducing physician isolation. Telehealth encounters increased 766% in the first three months of the COVID-19 pandemic, with sustained growth afterward. For physicians, telemedicine:
- Reduces professional isolation through virtual consultation and peer collaboration
- Provides access to specialist backup for complex cases
- Supports continuing education through virtual conferences and case reviews
- Signals that the organization is forward-thinking and technology-enabled
One rural hospital in Texas using a virtual team model achieved a 40% reduction in turnover and near-zero vacancy rates, demonstrating measurable recruitment and retention impact.
Professional Development Pathways:
Early-career physicians are motivated by growth. Build development into the role from day one:
- Establish formal mentorship structures for early-career hires
- Fund attendance at medical conferences annually
- Create leadership tracks: medical director pathways, committee roles
- Pursue academic affiliations where geography allows

Physicians weigh these opportunities as seriously as compensation — and they're far less expensive to deliver.
Community, Lifestyle, and the Full Relocation Picture
Physicians who experience social isolation or whose spouses cannot find fulfilling employment are likely to leave regardless of financial incentives. Community integration is a long-term retention factor, not just a recruitment talking point.
Recruit the Household, Not Just the Physician
Identify and communicate what is genuinely special about your community:
- Outdoor recreation (hiking, fishing, skiing)
- Local culture (arts, music, festivals)
- Cost of living advantages (housing affordability, low taxes)
- School quality (academic performance, class sizes, extracurriculars)
- Pace of life (less traffic, community connection, safety)
Structure Site Visits Around the Whole Family
Introduce candidates and their families to:
- Community members and local employers (for spousal employment)
- Real estate agents who understand relocation needs
- School administrators and teachers
- Local business owners and civic leaders
- Current physicians and their families
A well-structured visit answers the question candidates won't always ask aloud: can my family be happy here?
Build Tangible Support Infrastructure
- Partner with local employers to create a spousal employment network
- Establish housing assistance programs or partnerships with lenders
- Connect with schools to facilitate enrollment and tours
- Coordinate with local government on relocation logistics
These partnerships accelerate community integration and reduce the friction that causes families to leave within the first two years.
The Boomerang Physician Strategy
That infrastructure also strengthens your case with a high-value candidate pool: physicians who already know the region. Physicians who grew up in or near the area are more than twice as likely to remain in rural practice. Target candidates who relocated for training but retain community ties, framing the opportunity as returning to serve a community they already know. Reach them through:
- State medical society networks
- Medical school alumni databases
- Geo-targeted social media campaigns
Expanding Your Physician Pipeline: Non-Traditional Channels and Government Programs
Long-term recruitment sustainability requires pipeline development, not just vacancy filling.
Rural Education Pipeline:
Physicians with rural backgrounds are significantly more likely to practice rurally long-term. Those completing rural residencies are 2-3x more likely to practice rurally. Partner with regional medical schools to:
- Support rural clinical rotations (even a single rotation increases the probability of rural practice)
- Host residency placements
- Fund rural-focused curricula or track programs
- Establish academic affiliations that provide teaching opportunities for your physicians
Investments in rural health workforce programs demonstrate a return of $3.50 for every dollar spent.
National Health Service Corps (NHSC):
The NHSC provides loan repayment in exchange for a two-year service commitment at NHSC-approved sites in HPSAs. 84% of NHSC participants remained in an underserved area for at least one year after completing their service obligation, making this a viable long-term pipeline rather than a temporary staffing fix.
To leverage NHSC effectively:
- Ensure your facility is NHSC-approved
- Promote NHSC eligibility prominently in job postings
- Integrate NHSC messaging into your recruitment outreach
Conrad State 30 J-1 Visa Waiver Program:
This program allows J-1 foreign medical graduates to waive the two-year foreign residence requirement. In exchange, they commit to a minimum three-year service at a qualifying HPSA facility. Each state receives a cap of 30 waivers annually, opening a meaningful candidate pool for underserved specialties.
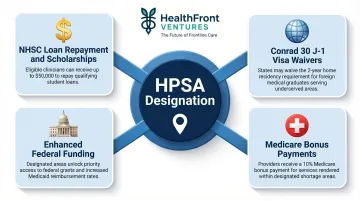
HPSA Designation:
HPSA designation is a prerequisite for accessing multiple federal recruitment resources. As of September 2023, 56.67% of all designated HPSAs were in rural areas. HPSA status unlocks:
- NHSC loan repayment and scholarship programs
- Conrad 30 J-1 visa waivers
- Medicare bonus payments
- Enhanced federal funding opportunities
If your facility qualifies, verify HPSA designation status before your next recruitment cycle — these benefits are available now.
Non-Traditional Candidate Channels:
Expand your recruitment funnel:
- Physicians pursuing financial independence and early retirement (FIRE) often seek meaningful short-to-medium-term assignments before stepping back
- Semi-retired physicians respond well to reduced-schedule rural roles that offer purpose without full-time commitment
- Locum-to-permanent pathways let candidates experience rural practice before committing to relocation
Each channel calls for tailored messaging. Lead with flexibility, mission, and lifestyle — not long-term career trajectory.
Frequently Asked Questions
How can a rural hospital attract physicians?
Lead with competitive compensation and loan repayment, then pair it with genuine lifestyle and professional autonomy advantages. Use a structured recruitment-for-retention process that prioritizes long-term match quality over speed of hire, involving the candidate's family and community partners throughout.
What financial incentives are most effective for rural physician recruitment?
The highest-impact incentives include:
- Loan repayment assistance
- Retention bonuses at 2-, 3-, and 5-year milestones
- Signing bonuses
- Housing or relocation support
No single incentive wins on its own. Transparency about the total package value — presented as a combined number — accelerates acceptance decisions.
What government programs help rural hospitals recruit physicians?
Three federal programs are most relevant:
- NHSC: Provides loan repayment for two-year service commitments
- Conrad State 30: J-1 visa waiver enabling international medical graduates to serve in HPSAs
- HRSA HPSA Designation: Unlocks access to multiple federal recruitment and funding resources
How does a physician's background affect their likelihood of staying in a rural area long-term?
Rural-origin physicians are more than twice as likely to practice in rural areas long-term. Rural clinical training during medical school or residency also increases the probability of rural practice by 2-3x, making pipeline and training partnerships a high-return recruitment strategy.
What role does telemedicine play in making rural positions more attractive?
Telemedicine reduces professional isolation, enables specialist consultation and peer collaboration, supports continuing medical education, and signals organizational modernity. It addresses one of physicians' most common concerns about rural practice while expanding the care the hospital can offer patients.


