
Introduction
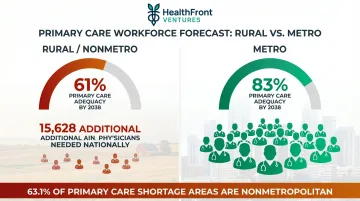
Physician networks face mounting pressure on two fronts: rising operational complexity and persistent workforce gaps, particularly in rural and underserved markets where analytics have shifted from a strategic advantage to an operational necessity. According to HRSA's 2025 State of the Primary Care Workforce report, 63.1% of primary care Health Professional Shortage Areas fall in nonmetropolitan regions — and 7.2% of U.S. counties have no primary care physician at all.
The healthcare analytics market is projected to reach $198.79 billion by 2033, yet most platforms were built for large urban health systems. Rural physician networks operate in a different reality: fragmented EHR environments, lean IT teams, and workforce retention challenges that standard tools were never designed to address.
This guide evaluates the leading healthcare analytics platforms for physician networks in 2026 — with a specific lens on how each performs for rural and underserved markets where the data stakes are highest.
TL;DR
- General health system analytics platforms frequently lack the physician network–specific capabilities that smaller and rural networks require
- Platform selection criteria: clinical data depth, physician network fit, EHR compatibility, value-based care support, and workforce analytics
- Health Catalyst and Arcadia lead for large multi-site physician networks and ACO arrangements; Epic Cogito is the lowest-friction option for Epic-native organizations
- HealthFront Baseline™ is the only AI-native solution purpose-built for rural physician networks, covering MD, NP, and PA workforce metrics with standardized rural county quality measures
- Matching the right platform to your network's primary use case is more important than chasing feature breadth
Why Physician Networks Need Dedicated Analytics Platforms in 2026
Healthcare analytics platforms in the physician network context are tools that aggregate, normalize, and deliver clinical, operational, financial, and workforce data to support network-level decisions. They differ from general business intelligence tools or basic EHR reporting modules by providing healthcare-specific data models, regulatory compliance frameworks, and clinical pathway intelligence that generic analytics cannot replicate.
The Fragmented Data Reality
Physician networks face distinct data challenges that set them apart from integrated health systems:
Fragmented EHR environments: The private practice share has declined to 42.2% in 2024, with many networks now spanning multiple EHR vendors across acquired practices. Standard reporting tools struggle to normalize clinical data when one practice runs Epic, another uses athenahealth, and a third relies on eClinicalWorks.
Value-based contract complexity: CMS approved 476 Medicare Shared Savings Program ACOs serving more than 11.2 million beneficiaries for 2025, with 53.4% of Traditional Medicare beneficiaries now in accountable care relationships. Networks managing shared savings distributions need real-time quality score tracking and risk stratification — capabilities standard analytics tools were never designed to provide.
Workforce availability gaps: Rural networks especially struggle with provider retention and recruitment. HRSA projects that 15,628 additional primary care physicians are needed to eliminate current shortages, with nonmetro areas expected to reach just 61% primary care adequacy by 2038, versus 83% in metro regions. Most traditional analytics platforms offer no workforce-specific intelligence to address that gap.
Each of these data challenges demands purpose-built tooling. The platforms below were selected based on maturity, physician network use case coverage, and demonstrated ability to convert fragmented data into decisions that move the needle on cost, quality, and workforce stability.
Best Healthcare Analytics Platforms for Physician Networks in 2026
Each platform below was evaluated against the same criteria to ensure consistent, comparable assessments:
- Data interoperability and EHR integration depth
- Physician network–specific use case coverage
- Value-based care readiness
- Pricing accessibility
- Support for both clinical and operational decision-making at the network level
Health Catalyst
Health Catalyst is an enterprise health data analytics vendor whose Data Operating System (DOS) aggregates clinical, financial, and operational data across a health system or physician network into a unified, normalized layer. The platform delivers seven core capabilities: Acquire, Organize, Standardize, Analyze, Deliver, Orchestrate, and Extend—providing a comprehensive data foundation without requiring organizations to build infrastructure from scratch.
For large physician networks, Health Catalyst brings three concrete advantages: pre-built analytics applications covering readmission risk, surgical outcomes, and population health; a strong track record with integrated delivery networks; and AI predictive models calibrated for performance benchmarking across provider groups.
The platform maintains SOC 2 and HITRUST certifications and has been recognized as a leader in population health management analytics by industry analysts.
| Aspect | Details |
|---|---|
| Key Features | FHIR-compatible data ingestion; pre-built clinical and operational analytics apps; AI-driven risk stratification; open workspace for custom analytics queries |
| Best Fit | Large multi-site physician networks and integrated delivery networks that need analytics at scale across multi-site networks without requiring in-house data infrastructure |
| Pricing | Custom enterprise subscriptions; contact vendor directly for physician network contract ranges |
Arcadia
Arcadia is a cloud-based healthcare analytics platform purpose-built for value-based care environments, with strong capabilities in ACO performance management, risk stratification, and payer-provider data connectivity. The platform was designed specifically to support the quality reporting and financial tracking requirements of Medicare Shared Savings Programs and commercial risk arrangements.
The practical differentiator for physician networks under value-based contracts is Arcadia's cross-system data aggregation — it pulls from both provider and payer sources in a way that makes shared savings distributions and quality score reporting operationally manageable rather than a manual lift.
Arcadia reports that MSSP ACOs using its platform earned nearly 20% higher average bonuses in 2022, totaling $279 million — though this represents vendor-reported performance rather than independent third-party validation.
| Aspect | Details |
|---|---|
| Key Features | Payer-provider data aggregation; risk stratification and care gap identification; quality measure tracking; ACO and Medicare Shared Savings program support |
| Best Fit | Physician networks and ACOs operating under value-based contracts, Medicare Shared Savings Programs, or commercial risk arrangements |
| Pricing | Custom enterprise pricing; contact vendor directly for mid-to-large physician organization contract ranges |
Optum Analytics
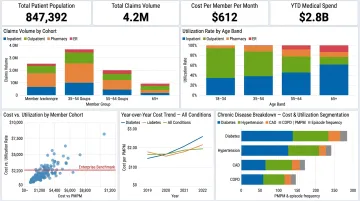
Optum Analytics is a UnitedHealth Group subsidiary with access to one of the largest longitudinal claims and clinical datasets in the U.S., offering population-level analytics capabilities that stand apart from pure platform competitors. The platform's EHR data asset covers more than 126 million unique lives with over 4.5 billion free-text medical notes, while its Clinformatics Data Mart claims asset spans more than 84 million lives across all 50 states.
For physician networks where financial and utilization analytics drive the primary objectives, Optum's scale is the deciding factor. The underlying data asset enables benchmarking, utilization outlier identification, and financial risk modeling that platform architecture alone cannot replicate.
The claims data has appeared in more than 300 publications over the past five years — a signal of research-grade depth that most analytics vendors cannot credibly claim.
| Aspect | Details |
|---|---|
| Key Features | Population-level claims analytics; cost and utilization benchmarking; financial risk modeling; chronic disease cohort identification |
| Best Fit | Physician networks and large provider organizations where claims-driven financial performance and population utilization analytics are the primary objectives |
| Pricing | Custom enterprise contracts; contact vendor directly for physician network implementation pricing |
Epic Cogito
Epic Cogito is Epic's native analytics layer, offering zero-ETL clinical reporting directly against live Epic data. SlicerDicer serves as the self-service cohort exploration tool, enabling clinical analysts and department administrators to build custom reports using keyword-based cohorting, drill-down to patient charts, and visualizations including bar charts, line graphs, maps, and treemaps.
For physician networks already standardized on Epic, Cogito removes the usual friction points entirely:
- No external ETL pipeline to manage or maintain
- No warehouse sync delay — dashboards reflect live EHR data
- No separate data infrastructure investment required
Epic's Population Health suite extends Cogito further, adding contract performance tracking, risk stratification, and social determinants of health tools designed for value-based care workflows.
| Aspect | Details |
|---|---|
| Key Features | Live Epic data reporting with no ETL delay; SlicerDicer self-service cohort exploration; pre-built clinical and operational dashboards; direct integration with Epic clinical workflows |
| Best Fit | Physician networks and health organizations fully standardized on Epic with limited multi-EHR complexity or cross-vendor data needs |
| Pricing | Enterprise licensing based on bed count and user volume; contact Epic directly for physician group deployment pricing |
HealthFront Baseline™ by HealthFront Ventures
HealthFront Ventures is an AI-native workforce data solutions provider specifically built for rural healthcare provider retention and recruitment. The company is launching HealthFront Baseline™ in Q1 2026 with FY25 Baseline Data Metrics covering MDs and NPs/PAs across rural physician networks.
HealthFront Baseline™ is the only platform in this list purpose-built around rural physician network workforce intelligence. Where every other vendor here addresses clinical or financial analytics, HealthFront targets a distinct gap: structured, benchmarkable workforce data for retention planning and provider recruitment incentive structuring.
The solution delivers four quantitative workforce metrics plus one rural county quality measure through a pre-built, outsourced AI data infrastructure. Rural health organizations get structured baseline data without commissioning custom builds. It is also EHR-agnostic, sourcing from external workforce and claims datasets rather than requiring EHR integration.
| Aspect | Details |
|---|---|
| Key Features | AI-native HCP Workforce Data Warehouses and Lakes; HealthFront Baseline™ with 4 quantitative metrics + 1 rural county quality measure; outsourced data infrastructure; focus on MD and NP/PA workforce tracking |
| Best Fit | Rural healthcare organizations, state-level Rural Health Transformation programs, and physician networks seeking structured workforce baseline data without building custom analytics infrastructure |
| Pricing | Contact HealthFront Ventures directly for pricing tied to FY25 Baseline Data Metrics availability beginning Q1 2026 |

How to Choose the Right Healthcare Analytics Platform for Your Physician Network
Avoid Common Selection Mistakes
Physician networks often make critical errors when selecting analytics platforms:
Brand recognition over use case fit - Choosing a nationally recognized vendor without confirming the platform addresses your network's specific analytical gaps leads to expensive shelfware and delayed time-to-value.
Underestimating integration complexity - A platform that cannot ingest data from your existing EHR vendors without heavy custom engineering will delay deployment by months and increase total cost of ownership by 30-50% through service fees.
Mismatched operational capacity - Selecting enterprise-scale solutions without first assessing your data engineering capacity creates ongoing dependency on expensive vendor services. That dependency compounds over time and erodes self-sufficiency.
Align to Primary Use Case First
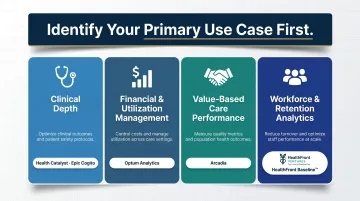
Before evaluating vendors, identify your single most critical analytical need:
Clinical depth - Temporal analysis, clinical pathway modeling, and outcomes measurement require platforms with structured clinical data models and longitudinal patient views. Health Catalyst and Epic Cogito excel here.
Financial and utilization management - Cost benchmarking, utilization outlier identification, and claims-driven performance tracking favor platforms like Optum Analytics with access to large comparative datasets.
Value-based care performance - ACO quality reporting, risk stratification, and shared savings distribution management require payer-provider data aggregation capabilities where Arcadia leads.
Workforce and retention analytics - Rural networks facing provider shortages need workforce-specific intelligence that tracks MD, NP, and PA supply, retention risk, and recruitment gaps—the domain where HealthFront Baseline™ is purpose-built.
Prioritize Data Interoperability and EHR Compatibility
FHIR compliance matters - ONC's Cures Act Final Rule and ongoing regulatory activities emphasize standards-based APIs, and nearly 9 in 10 hospitals enabled patient access via API in 2024. Platforms that support FHIR-based data ingestion reduce integration risk and technical debt compared to proprietary extraction methods.
Multi-vendor EHR environments - If your network operates multiple EHR systems across acquired practices, prioritize platforms with proven multi-vendor data normalization capabilities rather than single-vendor native solutions like Epic Cogito.
Assess Scalability and Implementation Capacity
Rural and smaller physician networks often lack the in-house data engineering teams that large enterprise platforms assume. The right platform should reduce the data preparation burden rather than add to it.
- Outsourced infrastructure options — Platforms offering managed data infrastructure or pre-built analytics frameworks let networks access advanced analytics without hiring specialized staff. HealthFront Baseline™ is explicitly designed as outsourced infrastructure for rural networks without internal claims processing capabilities.
- Implementation timelines — Ask vendors for deployment timelines specific to physician network environments, not hospital implementations. Networks with limited IT resources should prioritize platforms with accelerated onboarding and minimal customization requirements.
Conclusion
The right healthcare analytics platform for a physician network is defined by how cleanly it fits that network's clinical, operational, and workforce reality—not by feature count or brand name. A large multi-site network managing ACO contracts needs fundamentally different capabilities than a rural network struggling to retain primary care physicians.
Rural physician networks face a distinct set of data challenges that most enterprise analytics platforms were not designed to solve. Before committing to multi-year contracts, evaluate platforms specifically on rural workforce data capability, interoperability with smaller EHR environments, and implementation feasibility.
Those criteria point directly to purpose-built solutions rather than adapted enterprise tools. Physician networks ready to establish a data-driven baseline for workforce retention and provider recruitment can explore HealthFront Baseline™ by HealthFront Ventures, launching Q1 2026 with pre-built, AI-native rural HCP workforce data infrastructure that delivers measurable metrics without custom development.
Frequently Asked Questions
Which healthcare data analytics platforms are best for physician network management?
The best platforms depend on network size and use case. Arcadia and Health Catalyst serve large networks focused on value-based care and enterprise analytics; Epic Cogito is ideal for Epic-native organizations seeking low-friction reporting; and HealthFront Baseline™ targets rural networks prioritizing workforce analytics and retention planning.
What are the top data analytics companies for healthcare?
Leading names across the healthcare analytics spectrum include Health Catalyst, Optum, Arcadia, and Epic. Specialized platforms often outperform general vendors for specific use cases, particularly when networks face challenges like rural provider shortages or multi-payer value-based contract management.
What are the main types of big data analytics?
The four main types of data analytics are descriptive (what happened), diagnostic (why it happened), predictive (what will happen), and prescriptive (what action to take). In physician network contexts, descriptive analytics track utilization metrics, diagnostic analytics identify care gaps, predictive analytics forecast patient risk and provider attrition, and prescriptive analytics recommend staffing levels or intervention protocols.
What are the top EHR systems for physician networks?
The leading EHR platforms used by physician networks include Epic, Oracle Health (formerly Cerner), athenahealth, and eClinicalWorks. Analytics platform selection should align with the network's primary EHR to minimize integration complexity and maintain data fidelity across clinical reporting workflows.
What is the most popular value-based care model among healthcare organizations?
The Medicare Shared Savings Program (MSSP) ACO model is widely adopted among physician networks, with 476 ACOs serving more than 11.2 million beneficiaries in 2025. Platforms like Arcadia are built around MSSP's quality reporting and risk stratification requirements, making ACO alignment a key selection criterion for networks entering value-based contracts.


