
Introduction
Nearly 8.5 million Americans are enrolled in both Medicare and Medicaid as dual-eligible beneficiaries, representing 13% of the Medicare fee-for-service population but accounting for 26% of all Medicare FFS spending. For healthcare providers serving these patients, understanding how Medicare-Medicaid crossover claims work is critical — billing errors on this population directly expose revenue and put legally protected patients at risk of improper cost-sharing charges.
A Medicare-Medicaid crossover claim is a process where Medicare, after adjudicating a claim as the primary payer, automatically forwards the remaining cost-sharing data to Medicaid for secondary payment on behalf of dual-eligible beneficiaries.
When the process works, it eliminates manual billing and shortens payment cycles. When it breaks down, providers face delayed payments, revenue leakage, and incorrect charges to patients who have no legal obligation to pay.
This guide covers what crossover claims are, how the end-to-end process works, what billing requirements apply, and where the process commonly breaks down—so billing teams and revenue cycle managers can recover Medicaid payments without leaving reimbursement on the table.
TL;DR
- Medicare automatically forwards claims to Medicaid via the COBA program after paying its portion—providers typically don't file separately
- The CMS BCRC (Benefits Coordination and Recovery Center) manages routing using eligibility data to direct claims to the right payer
- Dual-eligible patients qualify for crossover only when Medicare is primary; Part C, Part D, and nursing facility claims are excluded
- Remittance codes MA18 and N89 confirm successful crossover; their absence requires manual Medicaid submission
- Submitting clean claims with correct NPIs, payer IDs, and secondary coverage data ensures successful crossover routing
What Are Medicare-Medicaid Crossover Claims?
A crossover claim occurs when a patient is "dual eligible"—enrolled in both Medicare and Medicaid. Medicare processes the claim first as the primary payer, pays its portion, and then electronically transmits the remaining cost-sharing obligations (deductibles, coinsurance, and copayments) to Medicaid for secondary payment. This eliminates the need for providers to file separate claims to Medicaid in most cases.
The infrastructure behind this process is managed by the CMS Benefits Coordination and Recovery Center (BCRC) through the Coordination of Benefits Agreement (COBA) program. COBA establishes a nationally standardized contract between CMS and Medicaid state agencies, assigning unique COBA IDs to each payer relationship.
The BCRC maintains a national repository of enrollment and eligibility data in the Common Working File (CWF). The CWF flags qualifying claims automatically, triggering the crossover transmission without additional provider action.
Crossover types to distinguish:
- Medicare forwards remaining balances to state Medicaid agencies for dual-eligible patients (Medicare-Medicaid crossover)
- Medicare forwards to private supplemental insurance plans for Medigap policyholders
- When Medicare is secondary to an employer plan, crossover does not apply
Not all Medicare claim types qualify for automatic crossover. Part C (Medicare Advantage) and Part D prescription drug claims are excluded — Part C claims are processed by private MA plans rather than Medicare Administrative Contractors, which places them outside the fee-for-service COBA workflow entirely.
Why Crossover Claims Matter for Healthcare Providers
Revenue Cycle Impact
Crossover claims directly affect a practice's financial health in two directions:
- When they work: Payment cycles shorten, accounts receivable aging drops, and Medicaid cost-sharing balances don't slip through as write-offs
- When they fail: Staff absorb manual resubmission work, cash flow stalls, and revenue leaks from claims that never reach secondary payer adjudication
Dual-eligible beneficiaries average $28,699 in per capita FFS Medicare spending annually, compared to $11,619 for non-dual beneficiaries—meaning these patients represent some of the highest-cost, highest-complexity claims a practice will process.
Compliance Dimension
Crossover claims are transmitted electronically with a documented trail, meaning both Medicare and Medicaid may audit the same claim. Accurate coordination of benefits documentation, correct eligibility verification, and proper claim coding are essential to avoid denials and compliance exposure under Medicare Secondary Payer rules.
Disproportionate Impact on Rural Providers
Rural providers serve a higher proportion of dual-eligible patients than urban practices. Approximately 20% of dual-eligible beneficiaries live in rural areas, compared to 16% of non-dual beneficiaries. With leaner billing staff, failed crossovers create disproportionate administrative strain for rural practices.
For rural organizations already managing thin administrative margins, this administrative load compounds workforce pressure — which is why tracking staff capacity against patient population complexity is increasingly part of rural health transformation planning.
How the Medicare-Medicaid Crossover Process Works
Understanding the crossover process helps providers catch errors before they turn into unpaid claims. It runs through four sequential steps: provider claim submission, automatic forwarding via COBA, Medicaid adjudication, and remittance review.
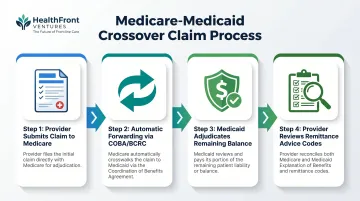
Step 1: Provider Submits Claim to Medicare
The provider submits a clean claim to Medicare using:
- CMS-1500 / 837P for professional services
- UB-04 / 837I for institutional claims
Medicare processes the claim as the primary payer, applying the applicable fee schedule and calculating deductibles, coinsurance, or copay amounts owed after Medicare's payment.
Step 2: Automatic Forwarding via COBA
Once the claim clears Medicare's processing cycle, the Medicare Administrative Contractor sends it to the BCRC. The BCRC combines claims by payer COBA ID and transmits them to the appropriate Medicaid state agency under the terms of that state's COBA agreement. The Medicare Remittance Advice (RA) will show code MA07 confirming transmission occurred — this code signals the claim has been forwarded to Medicaid for review.
Step 3: Medicaid Adjudicates the Remaining Balance
With the COBA transmission complete, Medicaid receives the crossover claim and pays the cost-sharing amounts Medicare did not cover, up to the Medicaid fee schedule limit. If Medicare's paid amount already exceeds the Medicaid fee schedule, Medicaid may pay little or nothing.
Some states also reduce the coinsurance payment when the Medicare-paid amount exceeds the Medicaid fee for certain provider types — check your state Medicaid agency's published rules to confirm how this applies to your claims.
Step 4: Provider Reviews Remittance Advice Codes
Once Medicaid adjudicates the claim, those results surface in the remittance advice codes. Providers should monitor for:
- MA18: Claim information forwarded to additional payer(s)
- MA07: Medicaid crossover indicator
- N89: Information forwarded to another payer from Medicare
If these codes are absent on the Medicare RA, the crossover did not occur and the provider must submit manually to Medicaid with the Medicare RA attached as proof of primary payment.
Billing Requirements and Claim Submission for Crossover Claims
Eligibility Verification
Providers must confirm Medicare is the primary payer and that the patient's Medicaid enrollment is active and current before submitting the claim to Medicare. Outdated or unverified eligibility data is the leading cause of crossover failures.
How to verify:
- Use HIPAA 270/271 eligibility transactions
- Check state Medicaid portals for current enrollment status
- Confirm dual-eligible status before claim submission
Claim Form and Data Requirements
Professional claims (CMS-1500 / 837P):
- Include the patient's Medicare ID
- Use correct payer sequencing (Medicare primary, Medicaid secondary)
- Ensure the NPI matches the NPI enrolled with the state Medicaid program
Institutional claims (UB-04 / 837I):
- Same NPI and payer sequencing requirements apply
- Mismatched NPIs cause the crossover to be rejected
Rate Codes and NDC Requirements
Enhanced Medicaid pricing:
Institutional providers receiving enhanced Medicaid rates (e.g., enhanced clinic rates) must include their Medicaid rate code on the Medicare claim in Loop 2300, HI Value Information segment (data element HI01 in the 837I format).
Part B drug reporting:
For physician-administered Part B drugs given to dual-eligible patients in outpatient settings, providers must report a 1-to-1 National Drug Code (NDC) for each Part B drug HCPCS code. Missing NDCs result in Medicaid denial of the crossover claim.
Manual Submission Fallback
When a claim is rejected from the BCRC crossover process due to data errors, the provider receives a notification letter with the claim control number and error explanation. In this case:
- Submit the claim directly to Medicaid manually
- Attach the Medicare Remittance Advice as proof of primary payment
- Consult your state Medicaid provider manual for submission instructions
Adjustment and Void Handling
- Adjustments: Submit directly to Medicaid using the standard adjustment process
- Voids: Submit to Medicare first — Medicare voids the claim and crosses over the voided transaction to Medicaid. Submitting a void directly to Medicaid for a claim that already crossed over will fail Medicaid's matching edits.
Common Crossover Claim Issues and When Crossover Doesn't Apply
Frequent Causes of Crossover Failure
Prevent failures by addressing these issues upfront:
- Register Medicaid enrollment data with the BCRC before submission
- Verify current Medicaid eligibility at each claim submission — not just at enrollment
- Confirm the NPI on the Medicare claim matches the NPI enrolled in Medicaid
- Check that your state Medicaid agency appears in the COBA trading partner directory
- Include all required fields, NDC codes, and rate codes on every claim

Automatic Forwarding Requires Provider Action
Automatic crossover still requires providers to do their part. Specifically:
- Verify Medicaid eligibility before submitting to Medicare
- Ensure correct claim data on the Medicare claim
- Monitor remittance advice codes to confirm crossover occurred
Providers who assume crossover happened without checking the RA codes risk losing Medicaid reimbursement altogether.
Claim Types Excluded from Automatic Crossover
The following claim types are not eligible for automatic COBA crossover and require manual submission:
- Medicare Part C (Medicare Advantage) claims
- Part D prescription drug claims
- Nursing home claims (providers must continue billing Medicare and Medicaid separately)
- Part B-only claims during an inpatient stay (must be submitted to Medicaid directly)
For these claim types, build a separate manual billing workflow rather than relying on COBA automation.
Primary Payer Rule
Crossover only applies when Medicare is the primary payer. If a patient carries active employer group health insurance, the employer plan takes primary payer status under these thresholds:
- 20 or more employees — working aged patients
- 100 or more employees — disabled patients
In those cases, the claim goes to the employer plan first; Medicare is secondary. The crossover process doesn't apply, and a standard MSP coordination of benefits workflow is required instead. Source: CMS MSP Employer Size Guidelines.
Zero-Paid Medicare Claims
If the Medicare deductible causes the Medicare payment to be zero, the claim still crosses over to Medicaid. Medicaid will cover the applicable deductible. A zero-pay Medicare claim still triggers the crossover process.
Conclusion
Medicare-Medicaid crossover claims, when properly managed, reduce administrative burden, protect revenue, and prevent erroneous patient billing for dual-eligible populations. The system depends on accurate eligibility data, clean claim submission, and active monitoring of remittance advice codes.
For providers serving dual-eligible populations—especially rural practices with high dual-eligible shares—the following competencies drive consistent Medicaid cost-sharing recovery:
- Understanding the COBA framework and how crossover claims route automatically
- Reading remittance indicators accurately to confirm or dispute coordination outcomes
- Recognizing exclusion categories that require manual submission
- Executing fallback procedures when automated coordination breaks down
Billing teams that build these workflows into standard operations recover what others routinely leave uncollected.
Frequently Asked Questions
What is a Medicare-Medicaid crossover claim?
A Medicare-Medicaid crossover claim is a claim Medicare automatically forwards to Medicaid after processing its portion of payment, on behalf of dual-eligible patients enrolled in both programs. This eliminates the need for providers to bill Medicaid separately for the majority of dual-eligible encounters.
Does Medicare crossover to Medicaid?
Yes, Medicare automatically crosses over claims to Medicaid for dual-eligible beneficiaries via the COBA program administered by the BCRC. However, crossover only occurs when Medicare is the primary payer and the patient's Medicaid enrollment is active and on file.
How long does a Medicare-Medicaid crossover take?
Once Medicare processes and pays its portion, the crossover transmission to Medicaid typically occurs within the same batch processing cycle. Medicaid's adjudication and payment posting timeframe varies by state and claim type, so providers should monitor both the Medicare RA and the Medicaid remittance.
What is the time limit for filing Medicare-Medicaid crossover claims?
Automatic COBA crossovers follow Medicare's processing cycle with no separate filing deadline. For manual submissions, state Medicaid timely filing limits apply — typically 90 days to 1 year. Florida allows up to 36 months from date of service or 12 months from Medicare adjudication; Texas requires 95 days from Medicare disposition.
How do I submit Medicare-Medicaid crossover claims to Florida Medicaid?
Florida Medicaid participates in the COBA crossover program, so most dual-eligible claims are forwarded automatically. When manual submission is required, submit directly to Florida Medicaid using the standard claim form with the Medicare RA attached and your NPI verified through the Florida MMIS portal.
What is the 80/20 rule for Medicare Part B and who pays the 20%?
Medicare Part B generally pays 80% of the approved amount for covered services after the annual deductible is met, leaving a 20% coinsurance owed by the patient. For dual-eligible beneficiaries, Medicaid covers this 20% coinsurance (subject to Medicaid's fee schedule limits), which is the cost-sharing amount that crosses over from Medicare to Medicaid.