
Introduction
The healthcare interoperability market is under pressure from every direction. Grand View Research projects the global market to reach $8.57 billion by 2030, up from $3.4 billion in 2023—a 14.15% compound annual growth rate. Three regulatory and operational realities are driving that growth in 2026:
- CMS interoperability mandates now taking effect across payer and provider networks
- ONC's HTI-1 Final Rule requiring certified health IT developers to adopt USCDI v3 by January 1, 2026
- Rural and underserved health systems catching up after being left behind in earlier digitization waves
Most healthcare organizations are still blindsided by the true cost. A simple FHIR API connection to a single system can run as little as $5,000, while full enterprise EHR deployments routinely exceed $1 million.
What vendor quotes rarely capture is what comes after: data migration complexity, annual maintenance that typically runs 15–20% of initial investment, and productivity losses of 8% or more in the first six months post-go-live.
This guide cuts through that ambiguity. It breaks down 2026 pricing tiers for EHR and FHIR integration, identifies the five factors that move costs up or down, and helps rural and small healthcare organizations budget realistically—without over-building for capabilities they won't need for years.
TL;DR
- FHIR API integrations start at $5,000–$50,000; full EHR data integration projects range from $30,000 to over $1 million
- Primary cost drivers: number of connected systems, integration method (FHIR vs. HL7 vs. middleware), organization size, and ongoing annual maintenance
- Rural clinics pay proportionally higher per-provider costs — large health systems offset this through volume pricing
- Pre-built, outsourced data infrastructure eliminates six-figure custom builds for rural clinics and state health programs
How Much Does Healthcare Data Integration Cost in 2026?
There is no single price for healthcare data integration. Costs depend on integration method, number of systems, deployment model, and your existing IT infrastructure.
This variability drives two common budget mistakes: organizations underbudget by focusing only on software licenses while ignoring implementation and training costs, or they over-specify for capabilities they won't need for years.
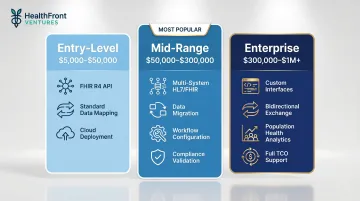
Typical Cost Ranges by Tier
Entry-Level: Single FHIR API Integration — $5,000–$50,000
Best for small clinics, telehealth startups, and rural health organizations connecting one or two data sources. Includes basic FHIR R4 API connection, standard data mapping, and vendor setup. Cloud-based deployment keeps infrastructure costs low.
Mid-Range: Multi-System EHR Integration — $50,000–$300,000
Designed for community hospitals, federally qualified health centers, and state-level rural health programs. Includes HL7 or FHIR integration across multiple platforms, data migration support, workflow configuration, and initial compliance validation for HIPAA and ONC requirements.
Enterprise: Full-Scale EHR Data Integration — $300,000–$1 million+
For integrated delivery networks, large hospital systems, and statewide digital health platforms. Includes custom interface development, bidirectional data exchange, population health analytics, and complete total cost of ownership commitments covering infrastructure, training, and long-term support.
These ranges cover project-level costs only. Budget separately for recurring expenses that most estimates leave out:
- Annual maintenance: 15–20% of the initial integration cost
- Staff training: approximately $1,200 per user at launch
- Compliance monitoring tools: ongoing cost that scales with system complexity
Key Factors That Drive EHR and FHIR Integration Costs
EHR and FHIR integration costs aren't fixed — they shift based on your technical setup, organizational size, and compliance obligations. For rural healthcare organizations in particular, a few of these variables carry outsized weight and are consistently mispriced at the planning stage.
Integration Method and Standard Used
Point-to-point custom HL7 v2 interfaces are labor-intensive and carry high long-term maintenance costs. FHIR REST APIs reduce custom development work by leveraging standardized resources and implementation guides, but require your EHR vendor to be FHIR-certified. Middleware and integration engine solutions sit between these two approaches—offering flexibility at higher upfront investment but lower long-term maintenance than custom HL7 builds.
The ONC HTI-1 Final Rule locks in FHIR R4 APIs and USCDI v3 as the baseline for certified health IT by January 1, 2026. Organizations prioritizing USCDI-aligned FHIR endpoints can reduce bespoke HL7 interfaces and avoid costly re-architecture when the next compliance cycle arrives.
Number of Systems and Data Flows
Each additional system connection—lab system, billing platform, radiology PACS, or population health tool—adds discrete interface development, testing, and support costs. One-way data flows (read-only) cost significantly less than bidirectional integrations that support both read and write operations. For example, some EHR vendors offer free one-way USCDI API export but charge for two-way Search and Create functionality— confirm current tiers directly with your vendor before budgeting.
Organization Size and Deployment Model
Cloud-based deployments shift capital costs to recurring subscription fees and reduce internal IT burden. On-premise deployments demand hardware investment and dedicated staffing. Per-provider pricing scales differently for a 5-provider rural clinic versus a 200-provider regional hospital. Rural providers consistently underperform urban peers on certified EHR adoption and Promoting Interoperability scores, often facing proportionally higher per-user costs due to smaller practice size and fewer resources for training and support.
Customization and Compliance Requirements
Standard EHR configurations rarely cover everything. Common scope-expanding requirements include:
- Custom workflow templates and specialty-specific data models
- HIPAA and ONC compliance validation and audit documentation
- State rural health transformation reporting — workforce metrics, quality measures, and utilization tracking
Each of these adds interface development time beyond what vendors quote in initial proposals.
Ongoing Maintenance and Support
Annual maintenance typically runs 15–20% of initial integration cost — for a $150,000 integration project, that's $22,500–$30,000 per year before any regulatory-driven changes. This recurring expense covers security patches, HL7/FHIR version updates, interface monitoring, and regulatory-driven changes. Build this line item into your initial budget — not as a contingency, but as a fixed recurring cost alongside licensing and staffing.
Full Cost Breakdown: One-Time and Recurring Expenses
Total cost of healthcare data integration goes well beyond the initial software fee. Understanding each cost category is essential for building a realistic multi-year budget.
One-Time Costs
Most organizations underestimate how many distinct line items appear before go-live. Three categories account for the bulk of upfront spend:
- Integration development — FHIR/HL7 interface builds, API configuration, custom data mapping, and vendor professional services. Entry-level FHIR API setups run $5,000–$50,000; complex multi-system HL7 interfaces can reach $100,000–$500,000.
- Implementation and go-live support — Project management, workflow validation, user acceptance testing, and go-live coverage typically consume 15–20% of total project cost. Phased rollouts reduce risk but extend timelines, so budget for extended project management during staged deployments.
- Data migration — Transferring years of patient records from legacy systems is the most underestimated line item. Simple single-system migrations run $5,000–$50,000; complex multi-system conversions with large data volumes can exceed $500,000 in enterprise environments.

Once the system is live, a separate set of costs begins — and they don't stop.
Recurring Costs
- Maintenance, support, and upgrades — Interface monitoring, security patching, FHIR version upgrades, and vendor support contracts typically cost 15–20% of initial integration investment per year. Organizations must budget for this annually to maintain system functionality and regulatory compliance.
- Staff training and change management — Initial training averages $1,200 per user, with ongoing training running $500–$1,200 per user annually. Inadequate training is the leading cause of implementation failure: industry surveys show only 38% of organizations rate recent EHR implementations as successful, with insufficient training quality among the top challenges cited.
Low-Cost vs. High-Cost Integration — What's the Real Difference?
A $10,000 FHIR API setup and a $500,000 custom EHR integration differ far beyond sticker price. The real gap is in capabilities, risk exposure, and how much flexibility you retain as your systems evolve.
Performance and Scalability
Lower-cost FHIR API integrations deploy quickly and work well for standardized, limited-scope use cases — connecting a single patient portal or a lab interface. Higher-cost custom HL7 or enterprise integrations handle complex, bidirectional workflows across regional lab networks, multiple billing platforms, and population health tools.
The tradeoff: enterprise integrations require extensive ongoing maintenance. Choose the approach that matches your actual workflow complexity, not the most technically impressive option available.
Compliance and Audit Readiness
Budget integrations may lack robust audit logging, granular access controls, and comprehensive HIPAA documentation. Premium implementations include end-to-end compliance architecture with automated audit trails, role-based access, and regulatory reporting. Compliance gaps discovered post-implementation can easily cost more to remediate than the original price differential.
Rural and resource-constrained organizations have a practical alternative: outsourced data infrastructure models that include compliance architecture by design — no remediation risk, no bolt-on fixes.
Long-Term Value and Vendor Lock-In Risk
Custom point-to-point integrations get expensive as your system grows. Key risks to weigh:
- Each new system connection requires additional custom development
- Switching vendors means rebuilding interfaces from scratch
- Accumulated custom code creates technical debt that compounds over time
FHIR-based and modular approaches reduce switching costs through standardized APIs. For organizations with limited IT staff, outsourced solutions that eliminate custom builds cut both technical debt and vendor dependency from the start.
How to Estimate the Right Budget for Your Organization
Budget estimation should start with organizational need, not vendor pricing. The right investment delivers reliable data exchange for your actual workflows—not the most technically impressive solution available.
Key Questions to Answer Before Budgeting
- How many systems need to connect?
- Is bidirectional data exchange required, or is one-way data flow sufficient?
- What compliance frameworks apply: HIPAA, ONC, state-specific reporting?
- Does your organization have internal IT capacity, or will you rely on a vendor or outsourced solution?
For Rural Healthcare Organizations and State-Level RHT Programs
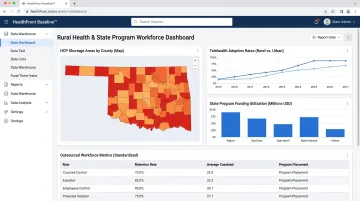
Pre-built, outsourced data infrastructure can eliminate the need for custom integration builds entirely. For example, HealthFront Baseline™ provides an outsourced HCP workforce data warehouse launching Q1 2026 with FY25 baseline metrics, replacing six-figure development projects with a structured workforce data platform that delivers standardized metrics without IT overhead. This approach allows rural clinics, FQHCs, and state programs to access analytics-grade workforce data without the infrastructure cost or staffing burden typically required to build it.
That cost-efficiency advantage matters most when you look at the full picture over time.
Factor in Total Cost of Ownership Over 3–5 Years
Include annual maintenance (15–20% of initial cost), training refreshers, and interface updates as FHIR and regulatory standards evolve. A $50,000 initial integration project becomes $80,000–$100,000 over three years when maintenance and training are included. Budget accordingly from the start to avoid surprises.
What Most Organizations Get Wrong About Integration Costs
Four planning mistakes consistently drive integration costs higher than necessary — and most are avoidable with earlier attention.
Budgeting only for year one. Annual maintenance, training, and interface updates commonly double the initial cost within three years. Organizations that plan only for launch often face funding shortfalls and deferred upgrades that compound technical debt over time.
Choosing price over long-term reliability. Skipping due diligence on FHIR compliance depth or a vendor's track record with similar-scale deployments leads to costly rework or failed audits. Verify USCDI v3 conformance, FHIR R4 alignment, and request references from comparable organizations before signing.
Underestimating go-live productivity loss. Research shows primary care practices experience roughly 8% declines in work RVUs and visits per FTE in months 1–6 after EHR implementation, narrowing to 4–5% by month 12. Net income per FTE can drop 16% initially. Build in extended floor support and plan for early revenue dips.
Attempting full-scope integration at once. A big-bang rollout sharply increases risk and cost compared to starting with core workflows and expanding incrementally. Phased approaches allow course corrections, reduce training burden, and give staff time to adapt before the next phase begins.

Frequently Asked Questions
What is the average cost of FHIR API integration for a small clinic in 2026?
Entry-level FHIR API integration for a small clinic typically ranges from $5,000–$50,000, covering basic FHIR R4 API connection, standard data mapping, and vendor setup. The key variable is the number of systems being connected and whether bidirectional data exchange is required.
How does FHIR integration pricing compare to HL7 interface costs?
FHIR REST APIs typically have lower custom development costs than HL7 V2 interfaces due to standardization and reusable implementation guides. However, long-term maintenance savings depend on your EHR vendor's FHIR certification depth, the number of systems involved, and confirmed USCDI v3 compliance.
Are there grants or funding sources to help cover EHR integration costs?
Yes. The Medicare Promoting Interoperability Program provides incentives for eligible hospitals and CAHs. HRSA offers rural health-specific grants that often include IT infrastructure funding, and state Rural Health Transformation programs explicitly support data sharing and technology investments. Verify current eligibility with program administrators.
What hidden costs should healthcare organizations budget for in a data integration project?
Data migration complexity, productivity loss during go-live (expect 5–10% throughput declines in months 1–6), custom interface development for non-standard systems, and ongoing annual maintenance that typically adds 15–20% of initial cost per year.
How long does a typical EHR or FHIR integration implementation take?
Simple FHIR API connections can deploy in a few weeks to two months depending on security review and testing. Full EHR implementations typically run 6–12 months for small to mid-size organizations, longer for multi-facility systems.
What is the difference between a one-time integration cost and total cost of ownership?
The initial project cost covers development, testing, and go-live support. Total cost of ownership includes 3–5 years of maintenance, security updates, staff training, regulatory compliance changes, and potential interface expansion—costs that typically dwarf the upfront investment.


